This blog explores real time data collected before and after the onset of COVID-19 across maternity services in England, drawing on PEP Health data, and CQC ratings, to reveal how PEP Health data supports the identification of variation in care experience. Our data uniquely provides proof that there is significant variation in care experience both between individual providers and for any given provider before and during the COVID-19 pandemic. Our insights into variation can be used to develop a real time and empirical early warning system, support resource allocation and encourage a learning system within the NHS.
Our insights show that the widest variation in care experience exists in London, the Midlands and the South East. We know that variation in care raises questions about the quality, health equity, and efficiency of resource allocation and use, and have important implications for health care and health policy. We encourage the use of real time data to support the empirical monitoring of variation in care experience in order to facilitate contemporaneous monitoring and safer and more respectful care and outcomes.
Our analysis can identify variation in real time, providing an opportunity to identify the providers that are deteriorating most rapidly across England and intervene in a timely and effective way.
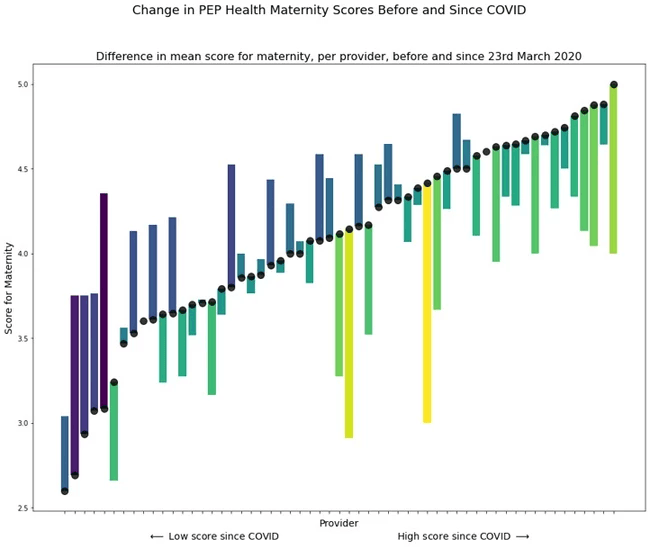
Figure 1: Difference in mean score for maternity, per provider, before and since COVID-19
Figure 1 illustrates the change in PEP Health maternity scores before and after the COVID-19 pandemic began. Here, each black dot represents a maternity service provider and the yellow and green bars indicate improvements in patient experience, the blue and purple indicate deteriorating patient experience. The longer the bar, the greater change in improvement or deterioration. This analysis reveals the five providers on the left-hand side have the lowest patient satisfaction scores and are significantly deteriorating in the COVID-19 environment. We also see that some providers have managed to significantly improve since the onset of COVID-19. Our data demonstrates evidence of deteriorating experience of care and should underpin the development of a real time data driven early warning system to monitor provider performance and enable genuine listening to patient feedback.
Crucially, we collect data across all services and all providers in England and the same methodology used to assess maternity services can be used to support peer-to-peer benchmarking of performance across any service, at any level (national, regional, departmental, ward etc.) and generate a ‘finger on the pulse’ of service provision to inform timely improvement strategies.
Next, we look at the variation of one provider in London in order to better understand how our data can be used as a real time indicator of the provision of safe, effective and dignified care.
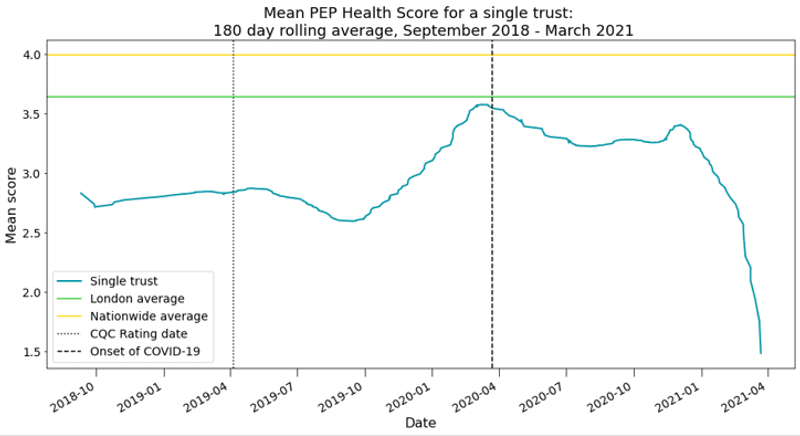
Figure 2: Mean PEP Health Score for an anonymized London Trust using the 180-day rolling average
This anonymized provider is located in a borough that experiences severe poverty and inequality, where more than 50% of children are deemed to live in household below the poverty line and boasts one of the highest ethnic minority populations. Compounding these variables with one of the worst performing maternity service scores in the country, the patient experience described through our insights is a rallying cry for support.
Key issues that are identified in the patient feedback reveal concerns for patient safety, inadequate access, poor communication between healthcare staff and patients and a dearth of respectful care provision. What is clear is that two years on from inspection, this provider has deteriorated to near critical levels, and our insights can be used as an early warning signal to the regulator to prioritize re-inspection. Furthermore, the feedback of the patients should be used to support a patient centered design of improvement strategies.
Our analysis into the variation in care across maternity services is timely. From the additional £100M NHS England funding recently announced to improve maternity services and staffing, to the Ockenden Report recommendations for maternity services and the recent announcement from Prof Ted Baker, the chief inspector of hospitals, to MPs that “38% of maternity services were deemed to require improvement for patient safety and some could get even worse” there is recognition that something needs to be done. Our data can support decision making, reduce risk, identify outliers and variation, support improvement and give a clearer, louder voice to the women and their families using these services.
If you would like to know how your maternity unit is performing and which aspects of care need to improve from the point of view of your patients, please contact enquiries@pephealth.ai.
